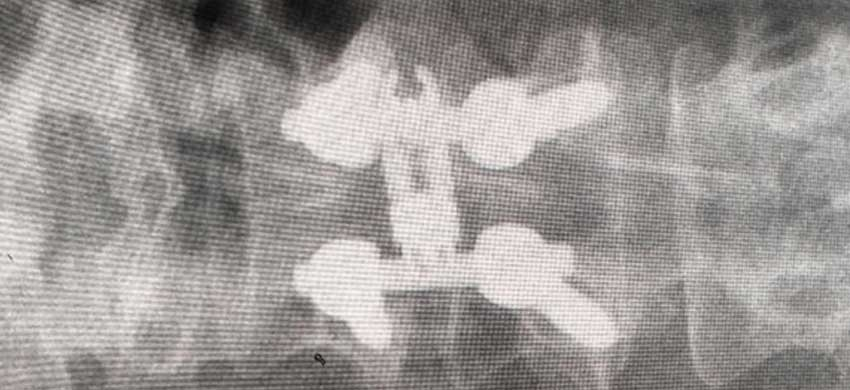
Lumbar Fusion
The spine support body’s weight and protects the spinal cord. It is agile and strong allowing for a wide range of movements. The spine is made of number of bones called vertebrae. They are connected to one another allowing spine to move and protecting the spinal cord and nerves. These strong interconnections are made up of intervertebral discs (which acts as shock absorbers) and facet joints (which connect one vertebra to another vertebra) and ligaments.
Why do I need a spinal fusion?
Spinal fusion is performed in patients who have back and/or leg pain. Sometimes the discs can lose their flexibility, elasticity and shock absorbing characteristics due to wear down, and with time can be a cause of back pain. There also may be instability due to excessive wear. In these instances spinal fusion will stabilize the disc and motion segment to help treat back pain. Sometimes surgery performed for leg pain (spinal decompression) will inevitably destabilize a spine motion segment, and is therefore backed up with a spinal fusion to prevent later problems.
What are the alternatives?
Back and leg pain symptoms may be treated with non-surgical methods for as long as possible. The treatment includes rest, ice or heat, weight control, exercise, physical therapy, medications and steroid injection. If these non-surgical treatments do not bring relief after a period of time, the doctor may recommend surgical treatment.
Who is suitable for spinal fusion for back pain?
- have ongoing lower back pain that limits their ability to perform every day activity at work or at home
- Fusion surgery for low back pain caused by degenerative disc disease is only considered on patients who
- have not had sufficient pain relief from extensive non-surgical treatment
- have received a diagnosis that a specific disc is the pain generator and other possible causes of low back pain have considered and ruled out Surgical options for spinal fusion
The surgery involves removal of the affected discs and fusion (joining the bones together). The spinal fusion is accomplished by bone growth between vertebrae, helping to minimize motion in the area, which my help reduce pain. This procedure can be used to treat a variety of conditions including disc herniations, asymmetric disc degeneration, nerve impingement, instability.
There are wide varieties of surgical procedures that can be performed to fuse the spine and the approach to the spine can also vary depending on the certain factors. It can approached from the
- side (Lateral lumbar interbody fusion)
- back (Posterior or Transforaminal lumbar interbody fusion)
- front (Anterior lumbar interbody fusion)
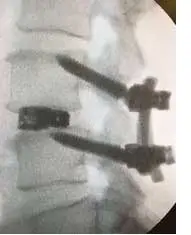 Posterior or Transforaminal Lumbar Interbody Fusion
Posterior or Transforaminal Lumbar Interbody Fusion
For these techniques, the surgeon will position the patient on their front, under general anesthesia. The reason to do PLIF vs TLIF is often dictated by the way your back has worn, or how the nerve are trapped. The main advantage of TLIF is that it can be done minimally invasively, so the surgeon can reach the vertebrae and intervertebral discs with minimal disruption of the nerves or muscles on the back.
Anterior Lumbar Interbody Fusion
In an anterior lumbar interbody fusion, the surgeon will position the patient on their back, under general anaesthesia. this is a less invasive surgery in which, the surgeon can reach the vertebrae and intervertebral discs through the abdomen. It is an option when patients have had multiple previous operations through their back.
Lateral Lumbar Interbody Fusion
In a lateral lumbar interbody fusion, the surgeon will position the patient on their side, under general anaesthesia. this is a minimally invasive surgery in which, the surgeon can reach the vertebrae and intervertebral discs without moving the nerves or opening up muscles on the back.
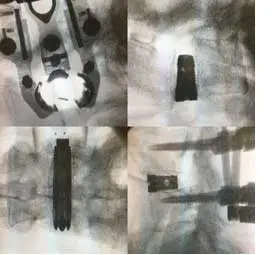 Surgical technique in general
Surgical technique in general
A appropriate incision in length is made (eg 2-4cms in TLIF). A special retractor will then be placed, through which your entire surgery will be performed. The retractor will be gently pushed through muscle until it reaches the spine. Then the surgeon will use special instruments to remove disc through this approach. As part of the fusion, the surgeon will stabilize spine by replacing the disc by a spacer.
This spacer is a cage made up of polymer plastic and/or titanium and filled with bone graft. The spacer relieves pressure from nerves and restores the disc height and provide stability to the spine for supporting normal loads. The instruments are then withdrawn the incisions are closed and dressed.
Benefits of surgery
- Less disability and better quality of life
- Improvement in low back pain and leg pain 12 months after the procedure
- Most patients (70% or more) are happy with the outcome of their procedure.
What are the possible risks or complications of this surgery?
Deep infection – approx. 1 in every 100 cases, you will be given antibiotics into the vein at the time of surgery to minimise this.
Superficial wound infections – 4 in every 100 patients get this and may require a short course of antibiotics.
Bleeding – less than 1 in every 100 patients have a significant bleed, which may require treatment.
Durotomy – the dura is the delicate sac that contains the spinal nerves inside the spinal canal. Occasionally, 1 in 25, this can become snagged or torn inadvertently during the surgery. This can usually be recognised and repaired at the time and would not cause any long term problems, You might have a headache for a couple of days afterwards.
Blood Clots – in the deep veins of the legs or lungs. You will be given surgical stockings and pumps on your legs during surgery to minimise this risk, although we cannot eradicate it.
Sensory change or muscle weakness in legs – is uncommon, approx 1 in 300, when it does occur, it is usually temporary but could be long-standing.
Post-op bladder or bowel dysfunction – The risk of damage to the nerves that supply your bladder and bowel is very rare, < 0.1% (1 in 1000).
Recurrence of Pain – In less than 1 in 100 people the natural process of healing by scar tissue causes pain to return by encasing nerves in too much scar tissue. This is treated by special medications.
Recurrent narrowing – is unlikely, and would take several years to develop.
Repeat surgery – 1 in every 100 patients have further back surgery during the ten years that follow due to continued back degeneration at other levels.
Back pain – Around 1-2 out of every 100 patients develop long term low back pain after spinal decompression, and this can often be treated non-surgically.
For elderly patients some risks are slightly increased. Risk of blood clots, heart attacks, urine/chest infection, and heart failure are all increased with advancing age.
Risks and complications
- Temporary nerve injury, damage to blood vessels, urinary tract infection, urinary retention and vertebral fracture, each in up to 1% of patients.
- Pain caused by damaged nerves in up to 5% of patients
- Problems affecting the digestive system in up to 7% of patients
- Problems with nerve function in up to 31% of patients, most of these were temporary
- Problems with the cage supporting the vertebrae, or the bone graft, in up to 3% of patients
- Infection or bleeding within the tissues in less than 1% of patients
- Another operation was needed in up to 6% of patients